The World Health Organization (WHO) has launched a new guideline1 that provides evidence-based recommendations to countries in their efforts to achieve control and elimination of schistosomiasis as a public health problem, and to move towards interruption of transmission.
“The main aim is to provide evidence-based recommendations to countries to eliminate schistosomiasis as a public health problem and to move towards interruption of transmission,” said Dr Amadou Garba Djirmay, who leads the global programme for the control and elimination of schistosomiasis. “The recommendations are designed to help countries in implementing national control and elimination programmes as well as verifying the interruption of transmission.”
The guideline can accelerate achievement of the target for the elimination of schistosomiasis as a public health problem and the interruption of transmission in humans in selected countries by 2030, as set out in the 2021–2030 road map for neglected tropical diseases. The six evidence-based recommendations for the elimination of morbidity and interruption of disease transmission in countries with high or low prevalence of the disease are:
- expansion of preventive chemotherapy to all in need, including adults and preschool-aged children;
- a single prevalence threshold to conduct preventive chemotherapy and its frequency;
- frequency of preventive chemotherapy (large-scale treatment) in transmission hot spots;
- safety of praziquantel for treatment of children aged 2 years and above, adults, pregnant women after the first trimester and lactating women;
- implementation of snail control as a strategy to reduce transmission;
- implementation of cross-sectoral approaches, including water, sanitation and hygiene (WASH); and
- diagnostic strategies for assessment of infection in humans, animals and snails and the environment.
The guideline, launched during a WHO-hosted webinar on 15 February 2022 (as part of World Neglected Tropical Diseases Day 2022 celebrations), marks an important milestone. It comes after years of progress and scale up of interventions made possible through the increased availability of donated praziquantel – the recommended medicine against all forms of schistosomiasis.
The WHO guideline on control and elimination of human schistosomiasis comes at a time when the global community is integrating approaches to tackle neglected tropical diseases. Initiatives include working closely with sectors such as WASH and One Health.
During the webinar, panelists spoke of the need to treat everyone – in both high and low prevalence settings. Discussion also focused on how to monitor and evaluate future integrated interventions that are crucial and the best methods that can be used to make informed decisions.
Vector and zoonotic control, and interventions aimed at treating all types of morbidities associated with schistosomiasis including female genital schistosomiasis, were discussed as well as advocacy, sustainability and domestic resource mobilization to sustain progress towards elimination.
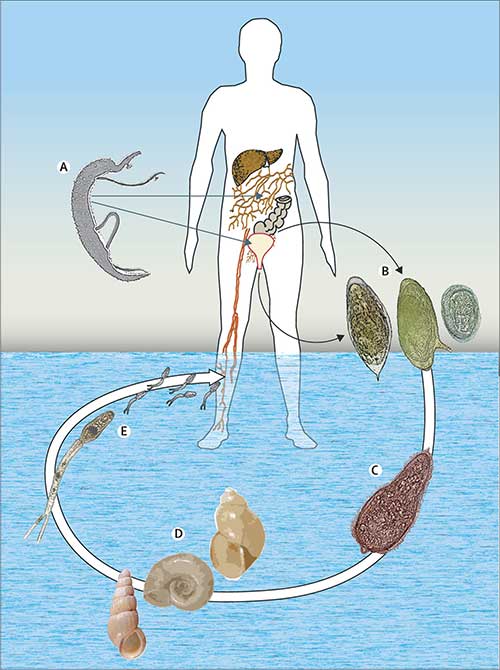
Schistosomiasis, also known as bilharziasis, is an acute and chronic parasitic disease caused by infection with blood flukes (trematode worms). The disease has been reported from 78 countries.
People become infected during routine agricultural, domestic, occupational and recreational activities, which expose them to infested water. Lack of hygiene and certain recreational habits of school-aged children such as swimming or fishing in infested water make them especially vulnerable to infection.
1 A WHO guideline is any document that contains recommendations for clinical practice or public health policy. A recommendation tells the intended end-user of the guideline what he or she can or should do in specific situations to achieve the best health outcomes possible, individually or collectively. It offers a choice among different interventions or measures having an anticipated positive impact on health and implications for the use of resources.
Recommendations help the user of the guideline to make informed decisions on whether to undertake specific interventions, clinical tests or public health measures, and on where and when to do so. Recommendations also help the user to select and prioritize across a range of potential interventions.